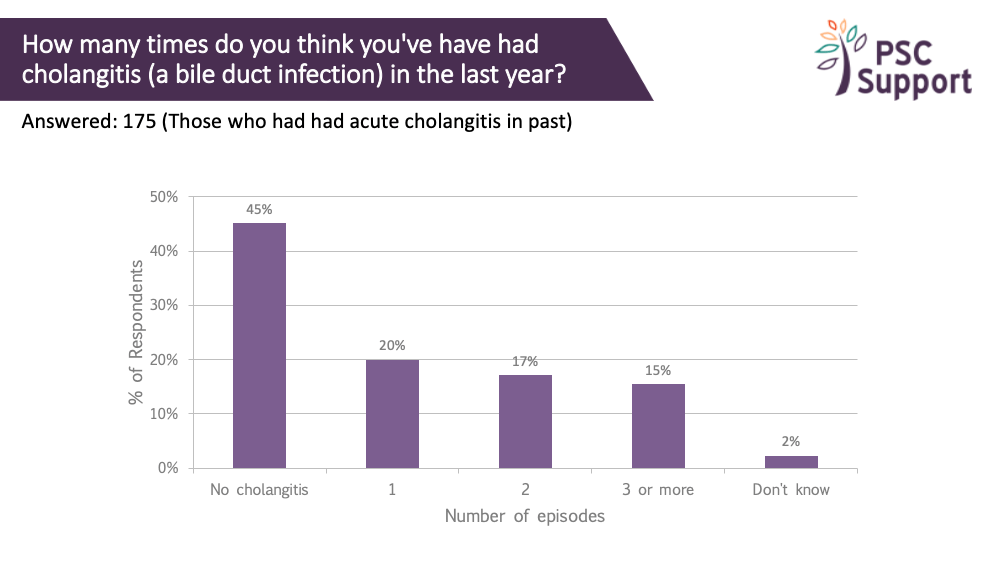Last year, you responded to our PSC Support survey to help shape PSC research design. Thank you to everyone who took the time to give answers. Your responses were (and continue to be) very helpful in our work with researchers to help improve how research trials are designed.
We shared the responses to the individual questions immediately after the survey closed, and now are working on the analysis and full report, which we've split into two parts, the first of which is available now:
Part 1 is about PSC healthcare (below).
Part 2 is about attitudes to research and study design.
Patient Insights Report
Part 1 - PSC Healthcare
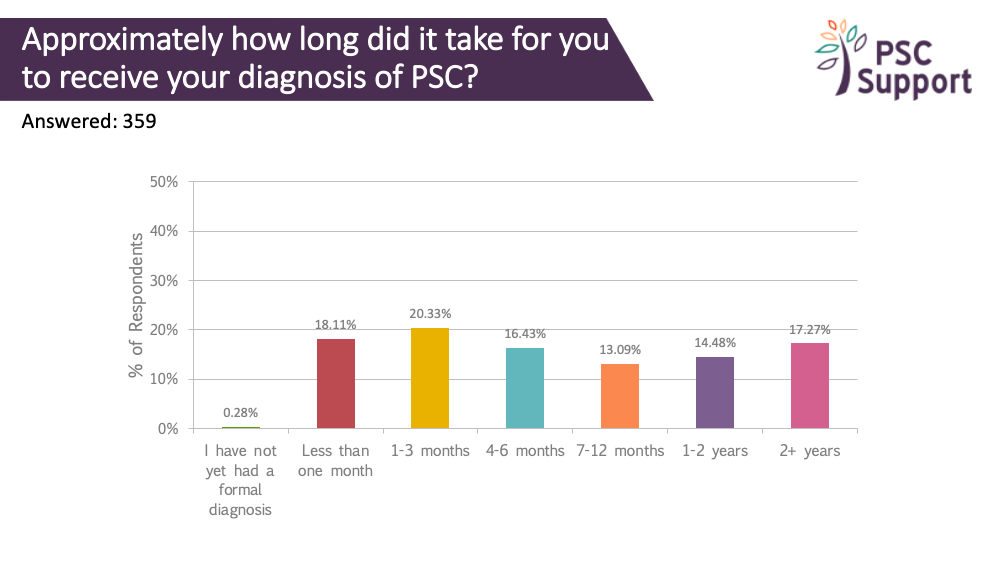
Less than a third (28%) of the 359 respondents reported that it took three months or less to be diagnosed with PSC. For one in six people (17.27%), it took more than two years to be diagnosed.
There is no single blood test to diagnose PSC, and doctors must put together clues from blood tests, scans and sometimes even biopsies. The lack of a definitive diagnostic test for PSC causes uncertainty, anxiety and stress for patients, delays important cancer screening and opportunities to take part in clinical trials.
People with PSC need a simple, definitive diagnostic test.
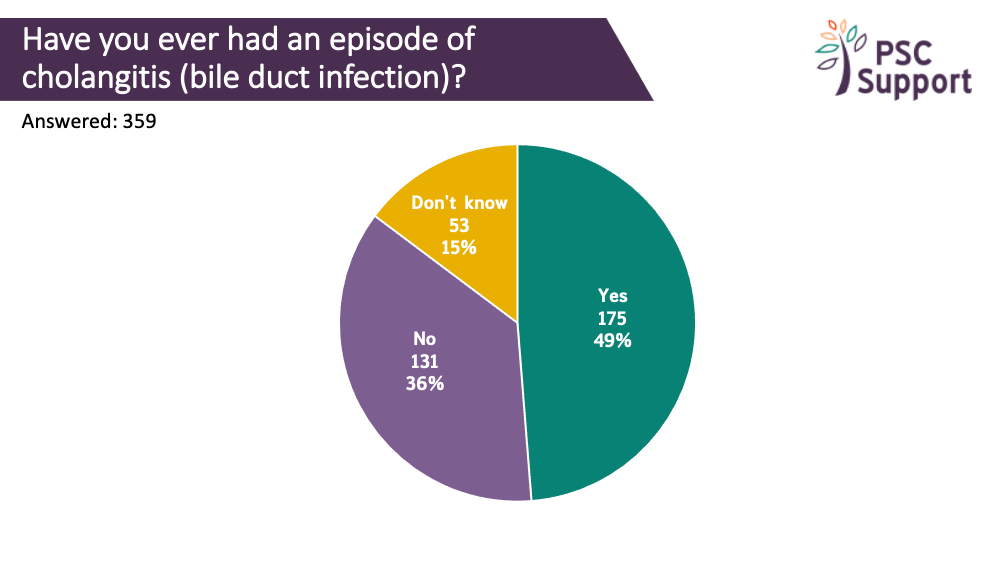
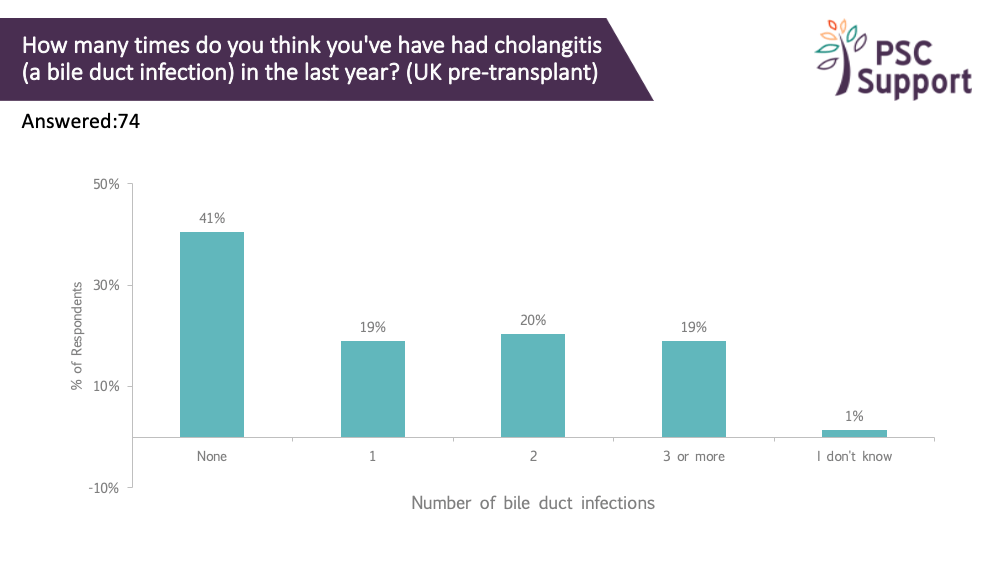
Cholangitis attacks in the last year
Half (49%) of the respondents had experienced a cholangitis attack and half of those (52%) had had one in the previous year. A third of these had had two or more cholangitis attacks in the previous year. Cholangitis attacks can appear out of the blue and are not necessarily an indication of progression. However, they do need urgent medical attention yet are not always easy to spot.
PSC Support and UK-PSC have developed an Alert Card to help patients and doctors understand and treat acute cholangitis attacks.
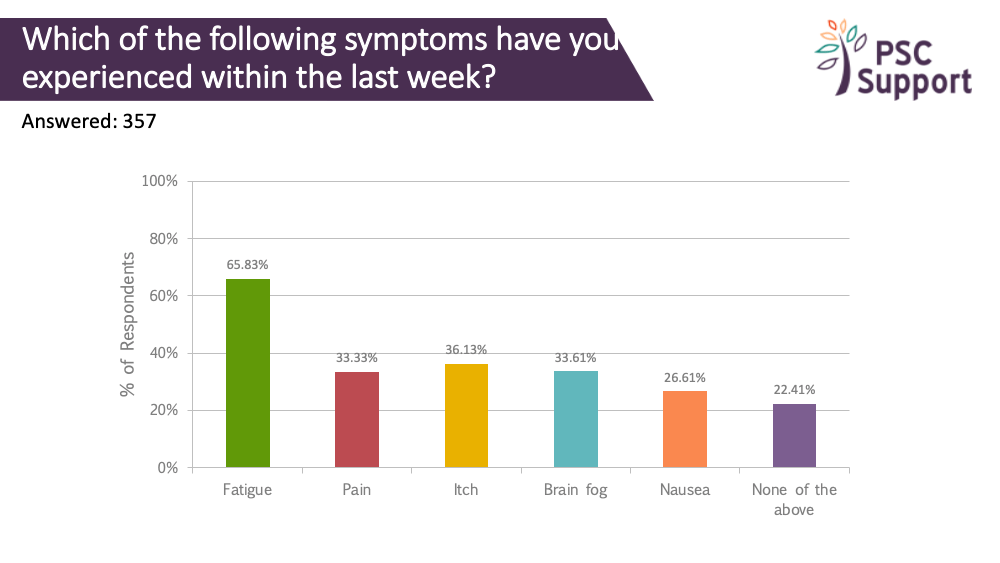
Symptoms in the last week
We've shown in previous surveys that people with PSC live with daily, invisible symptoms. In this survey, two in three people (66%) indicated that they had had fatigue in the previous week, and one in three suffered with itch (36%), brain fog (34%), pain (33%) and nausea (27%). PSC affects people at any age, and many are raising young families and trying to hold down jobs. These symptoms can be debilitating and seriously affect quality of life and ability to work.
People with PSC urgently need effective treatments to manage all these symptoms, as well as to stop progression of the disease.
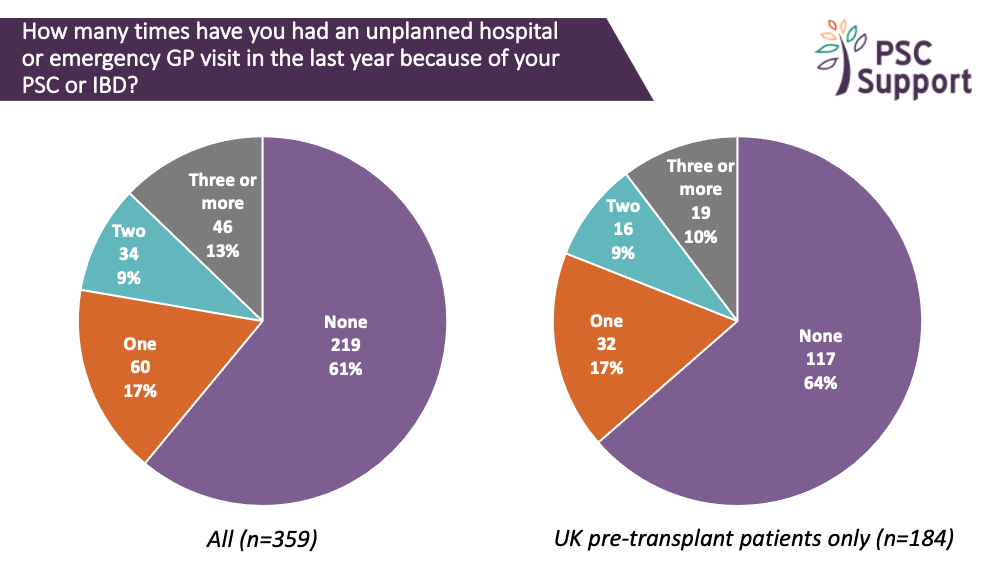
Emergencies in the last year
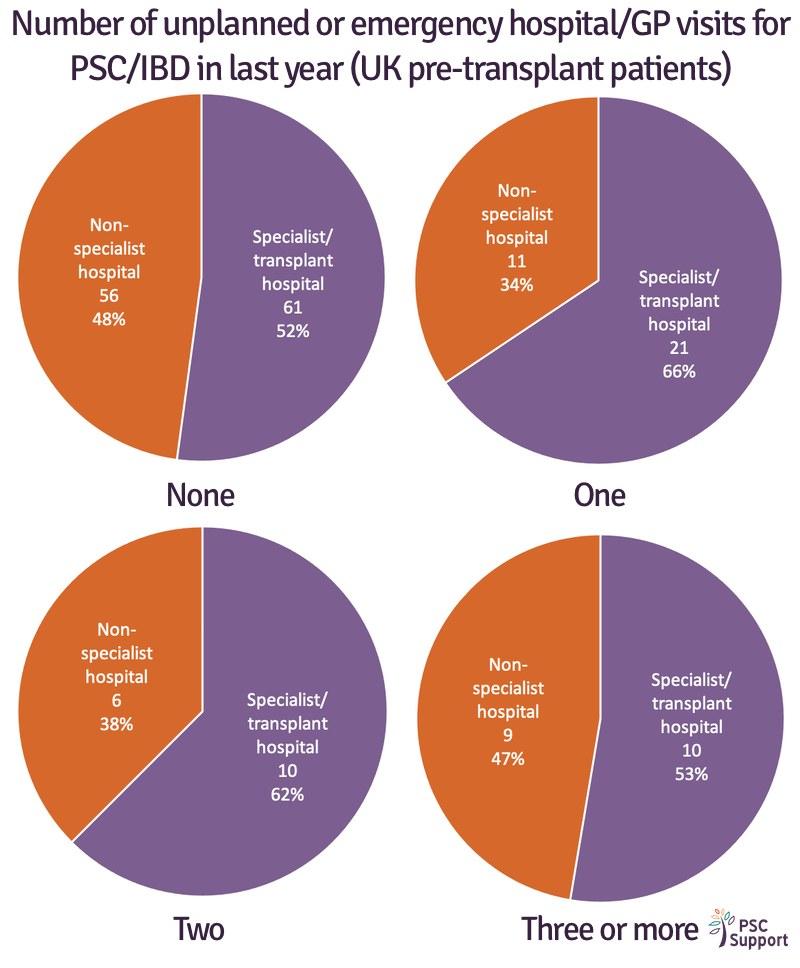
PSC is an unpredictable disease, and for some, causes frequent, unexpected emergencies. More than one in three respondents had had an unplanned hospital or emergency GP visit for PSC or IBD in the previous twelve months.
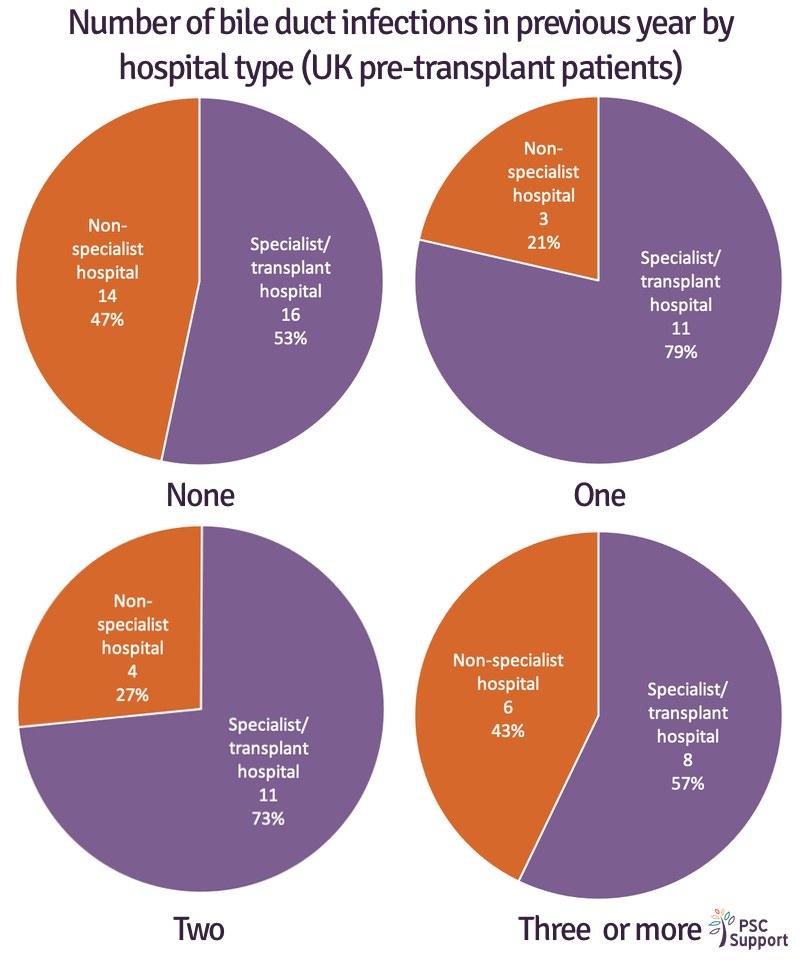
In the UK, one in ten (10%) patients had had three or more unplanned hospital or emergency GP visits yet surprisingly, nearly half (47%) of those patients were being cared for general clinics.
It is important that when patients start to experience complications, their care is discussed by a team with experience and expertise of PSC complications.
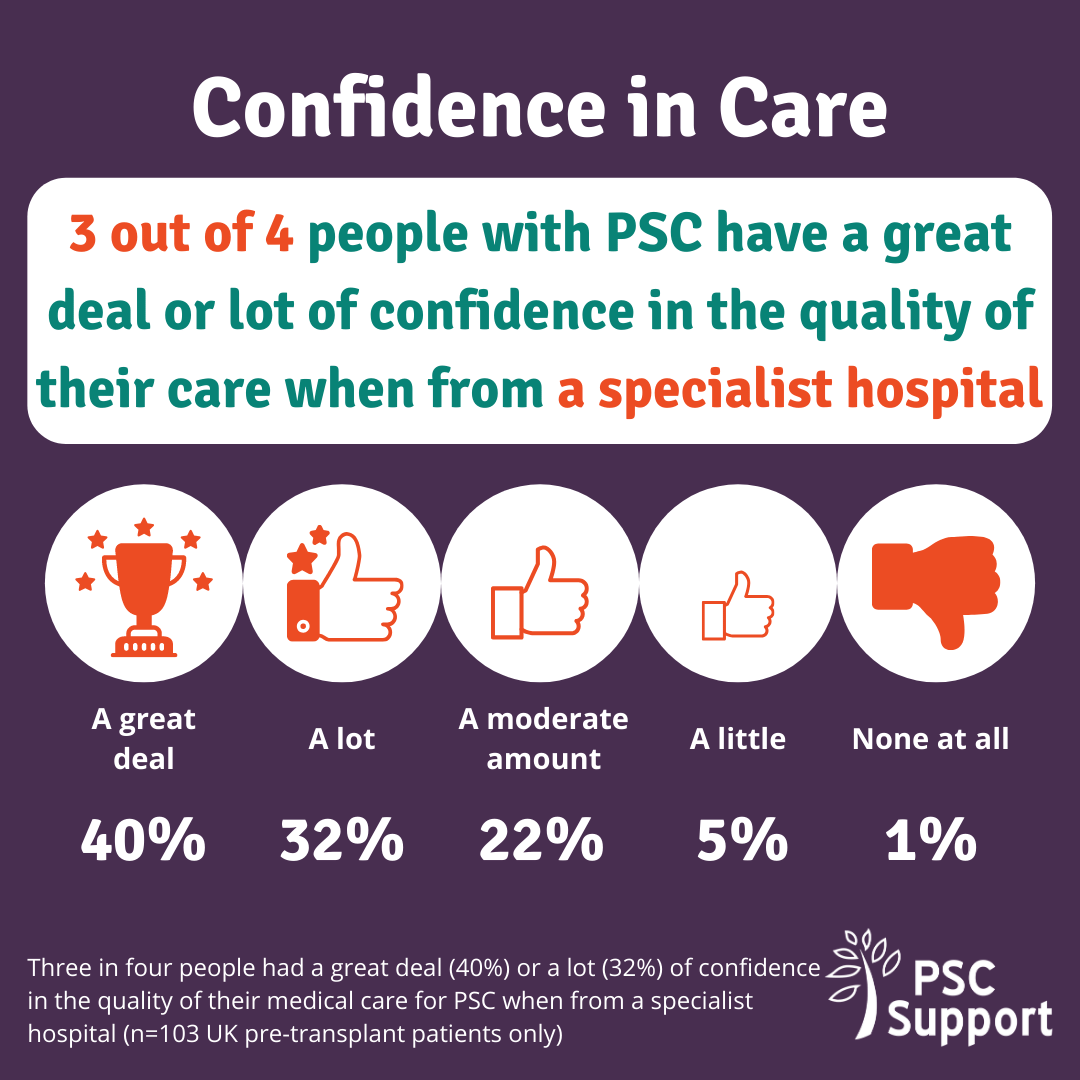
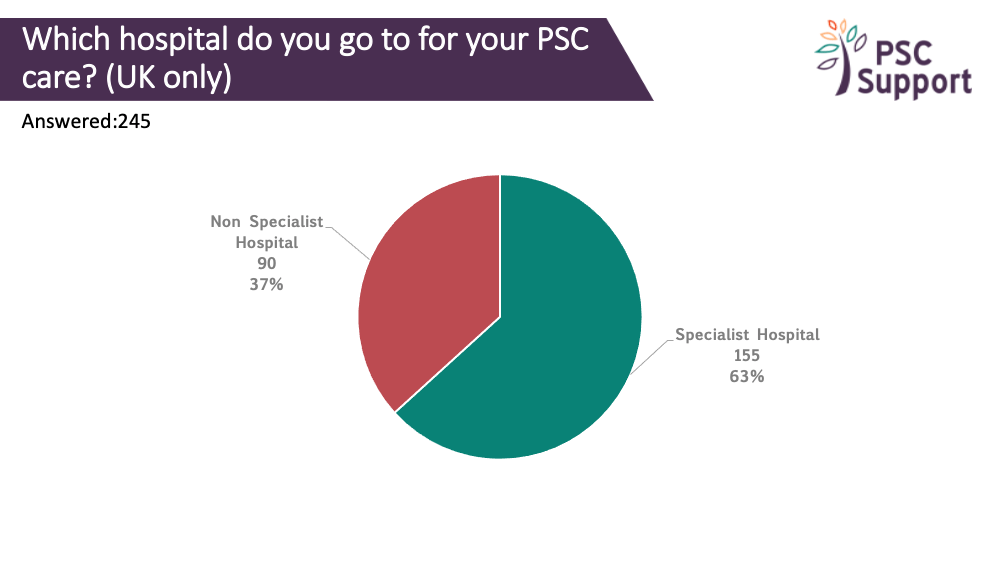
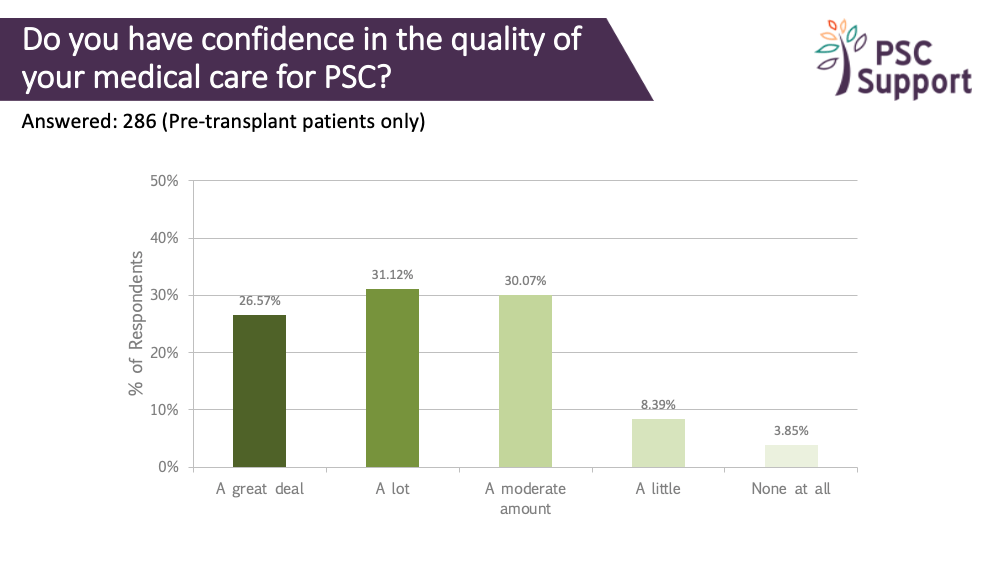
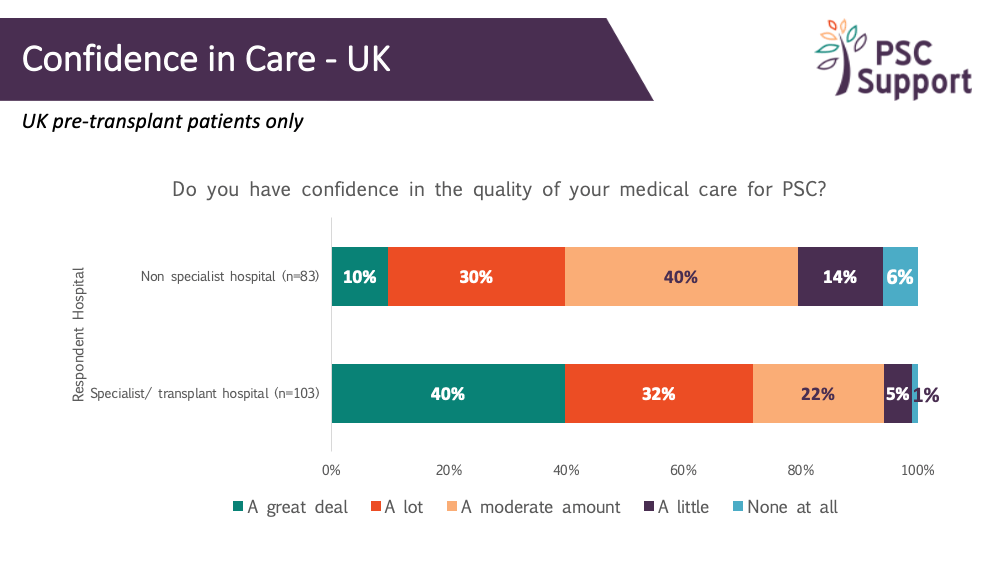
Confidence in Care
Overall, only a quarter of respondents had a great deal of confidence about their medical care for PSC. We looked more closely at the responses of UK patients who had not had a transplant. Not surprisingly, confidence was far greater for those being seeing specialist hospitals, with 40% having a great deal of confidence and another 32% having a lot of confidence. In non specialist hospitals only 10% had a great deal of confidence and 20% had a lot of confidence in the quality of their care.
UK-PSC published new guidelines for the management of patients in 2019. PSC Support worked with UK-PSC to develop the guidelines. This year, we are providing patient representation to develop new European-wide guidelines to manage PSC.
Greater awareness of the PSC guidelines is needed. We are working to raise awareness of these guidelines with patients and healthcare professionals who care for people with PSC.
PSC Support Patient Insights Survey (Part 1 - Living with PSC) was written by PSC Support and published 05 May 2020. www.pscsupport.org.uk/insights-living-with-psc